Tuberculosis is an ancient infection, and while it is thought to be significantly older, evidence of TB has been found in human remains from the Neolithic era. Tuberculosis was impacting societies when Herodotus was writing his Histories and the pyramids were under construction. The Old Testament even describes a chronic and wasting lung infection that is strikingly similar to TB (1). For much of our history, this infection has been uncontrollable and surrounded by mystery, a sickness to be both feared and romanticized.
Prior to the late 19th century, theories of transmission and protocols for the treatment of TB were varied and, in many cases, wholly incorrect. The touch of a king, herbal concoctions, and bloodletting were all once considered viable cures (2).
Death by TB was even considered a fashionable and romantic way to perish. A drawn out death from ‘consumption’ featured heavily in the literature and arts of the era. The morbid romanticism surrounding the disease was so powerful that some ladies would even powder their faces to attain the striking pallor of a fading TB victim (ibid). At one point, tuberculosis was thought to be associated with and even caused by vampires! Malaria never became quite so fashionable.
The onset of the Industrial Revolution and the flood of immigration into increasingly overcrowded, poverty-stricken urban centers provided the ideal environment for increasingly rapid TB transmission. TB began to be widely associated with the characteristic evils of poverty. By the late 1800s, 1 out of 7 people in Europe died from TB.

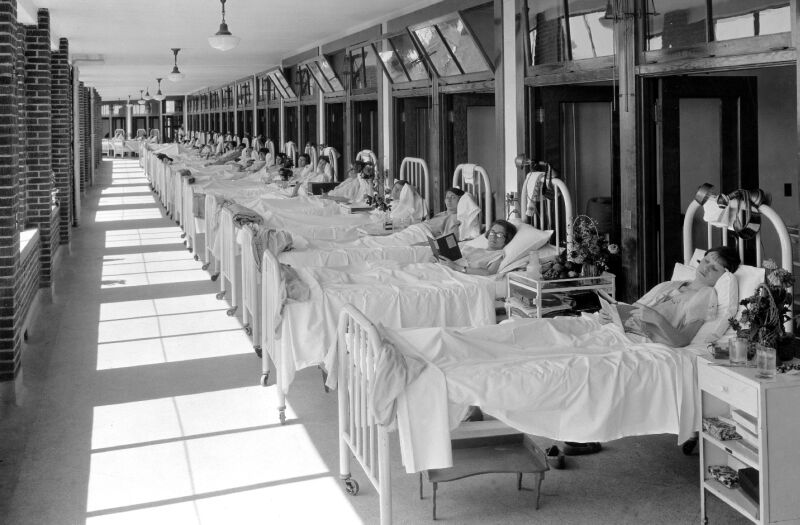
Finally, on March 24th, 1882 (Today, this date is acknowledged globally as World TB Day) Robert Koch announced the successful isolation and identification of Mycobacterium tuberculosis, the causative agent of the disease. Despite knowing the etiological origin, antibiotic treatments were nonexistent. Treatment strategies focused on separating sufferers from the general population, improving nutrition, and alleviating environmental conditions that posed a high risk for transmission.
Another 60 years passed until an antibiotic was finally identified that could successfully fight this uniquely resilient infection. The next 3 decades that followed brought new waves of drug therapies, which when used in combination, significantly reduced the length of treatment and decreased mortality. It was an exciting time in the control of TB. More people were being treated and cured and the rapid progress suggested that the control of the infection was within reach.
However, after millennia of not-so-peaceful coexistence with humanity, TB was not going to be so easily defeated. Drug resistant strains appeared, which hampered the success of treatment (3). Then, most significantly, the global HIV epidemic erupted, providing TB with a growing reservoir of people with weakened immune systems vulnerable to a co-infection like TB (Read more about HIV/TB coinfections here). By 1993, the World Health Organization had declared the TB epidemic to be a global health emergency.

By 1995, the WHO rolled out DOTS (directly observed therapy, short course); a multifaceted strategy focused on increasing cure rates and limiting the spread of drug resistant TB in high incidence areas. The strategy put into place centralized case and treatment reporting protocols, standardized monitoring and evaluation, and promoted the daily provision of TB treatment to sufferers by a network of medical professionals and community health workers (4). DOTS was widely adopted and is considered one of the most successful WHO control strategies, despite the demands this resource intensive approach can place on governments and weak health systems.
After almost two decades of prioritizing DOTS, progress has been made, although HIV/TB coinfection and TB resistance continues to persist, particularly in areas with overburdened or non-existent medical networks (5). Additionally, limitations in our technological capacity to quickly and effectively diagnose TB have hampered efforts to identify and treat TB cases (6).
However, despite these complex challenges, by better understanding the limitations of current approaches and advocating for unwavering commitment to the global control of TB, steady progress can continue to be made. A greater commitment from governments to universally extending access to testing and increasing funding for health services will improve case detection among the most vulnerable and high-risk populations. In addition to these frontline, treatment-focused strategies, the private and public sectors need to begin to prioritize prevention of TB infection within these particularly high-risk communities. Such approaches could protect the hard fought and hard won advances and reduce the long-term need for costly subsequent health interventions.
-Olivia Johns; Research Officer
